Postexposure prophylaxis (PEP) is a type of medication that can help prevent HIV from developing in people who may have experienced exposure to the virus.
A person can get PEP after speaking with a healthcare professional or visiting the emergency room or an urgent care clinic. Some pharmacies can also provide PEP.
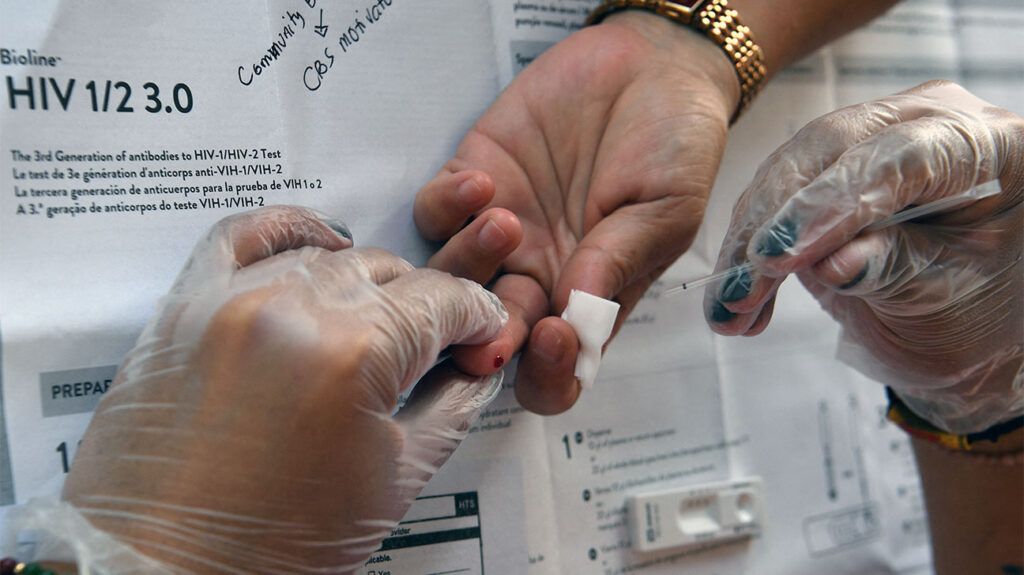
PEP is an antiretroviral medication regimen that prevents a person from developing HIV after experiencing exposure to the virus.
“Prophylaxis”
The
PEP is only for emergency situations after a possible exposure to HIV. Preexposure prophylaxis (PrEP) is an option for those who may experience frequent exposure. A person can speak with a healthcare professional about whether PrEP is the correct choice for them.
PEP vs. PrEP
PrEP is another type of medication to help prevent HIV.
The main difference between PEP and PrEP is when someone takes the medication. A person takes PrEP before a potential exposure to HIV, while PEP can help prevent HIV after a person has experienced exposure.
A healthcare professional may prescribe PrEP to those who have an increased risk of exposure through sex or using injected drugs.
A person may require PEP if they do not have HIV or are unaware of their HIV status and may have experienced an exposure to HIV within the last 72 hours (3 days).
Some scenarios that can result in a person needing PEP include:
- a condom breaking during sex with a partner with a positive or unknown HIV status
- using a shared needle, syringe, or other equipment to inject drugs
- a possible workplace exposure, for example, a needlestick injury
- having experienced sexual assault
PEP is effective in helping prevent HIV. Taking PEP consistently and correctly can reduce the risk of contracting HIV by 80% or more.
It is important that people use other prevention methods while taking PEP to help prevent transmitting the virus to others.
This can include using condoms and other barrier methods of protection during sexual activity. For those who use injected drugs, it is important to only use new, sterile needles and syringes.
There are
The preferred course of treatment involves taking 300 milligrams (mg) of tenofovir disoproxil fumarate and 200 mg of emtricitabine once a day, alongside 400 mg raltegravir twice a day, or 50 mg dolutegravir once a day.
An alternative course is taking 300 mg of tenofovir disoproxil fumarate and 200 mg of emtricitabine once a day, alongside 800 mg darunavir and 100 mg ritonavir once a day.
Follow-up care
A person will need to attend follow-up appointments to test for HIV after 4 to 6 weeks and again at 3 months after possible exposure.
A person who thinks they have experienced exposure to HIV should immediately contact a healthcare professional or visit an emergency room or urgent care clinic.
A healthcare professional will evaluate the person and help them decide if PEP is the correct course of action.
The World Health Organization has updated its guidelines to allow further access to PEP. The guidelines now include:
- community-based delivery to provide PEP closer to where people live, ensuring more timely access
- nonspecialist healthcare workers, such as pharmacists, being allowed to prescribe PEP
People can use HIV.gov’s online tool to find PEP services near them.
PEP is safe. However, a person should tell the healthcare professional prescribing PEP if they:
- are taking any medications
- have kidney problems
- are pregnant or nursing
Although PEP is safe to take while pregnant or nursing, it is important to tell the healthcare professional so they can decide on the best PEP regimen to follow. PEP may also interact with certain medications.
A person may experience some side effects from PEP,
These side effects are temporary and
In many states, insurance is likely to cover the cost of PEP. People who do not have insurance can access patient assistance programs (PAPs), which some pharmaceutical companies offer to help people get medications at a reduced cost or for free.
Pharmaceutical companies may also offer copayment assistance programs (CAPs) to help those with insurance to lower the cost of copayments, deductibles, or coinsurance for some medications.
These PAP and CAP requests can be handled urgently, and the healthcare professional who prescribed PEP may be able to help fill out the forms.
Those who require PEP as a result of sexual assault may qualify for a partial or total reimbursement of both the medicines and clinical care costs. People can find out more through the Office for Victims of Crime, which the Department of Justice funds.
If a person experiences HIV exposure at work, workplace health insurance will usually cover the cost of PEP.
What should I do if I think I have been exposed to HIV?
If a person thinks they have experienced exposure to HIV, they should contact a healthcare professional immediately or quickly visit an urgent care clinic or emergency room. A healthcare professional will evaluate the person and prescribe PEP if necessary.
How can a person lower their risk of exposure to HIV?
To lower the risk of HIV exposure, people should:
- use barrier methods of protection during sex
- avoid injecting drugs, and only use sterile injection equipment if they do use injectable drugs
- take antiretroviral therapy if they have a positive HIV status
What happens if PEP does not work?
Although PEP is highly effective, a person
There is currently no cure for HIV, but treatment can help:
- reduce a person’s viral load
- prevent the virus from transmitting to others
- prevent drug resistance
In most cases, treatment can manage the condition within
Postexposure prophylaxis (PEP) is a type of antiretroviral medication that a person takes after experiencing exposure to HIV. The medication helps prevent HIV from establishing an infection in the body.
PEP works best if a person takes it within 72 hours (3 days) of exposure to HIV, but ideally within 24 hours. If a person thinks they have experienced exposure to HIV, they should immediately contact a healthcare professional or visit an urgent care clinic or emergency room.
They will need to take PEP for 28 days and then attend follow-up appointments after 4 to 6 weeks and 3 months. At these appointments, a healthcare professional will test the person for HIV.

